A Hong Kong man got the new coronavirus twice
In the first confirmed case of reinfection, the man only got sick during his first round with the virus
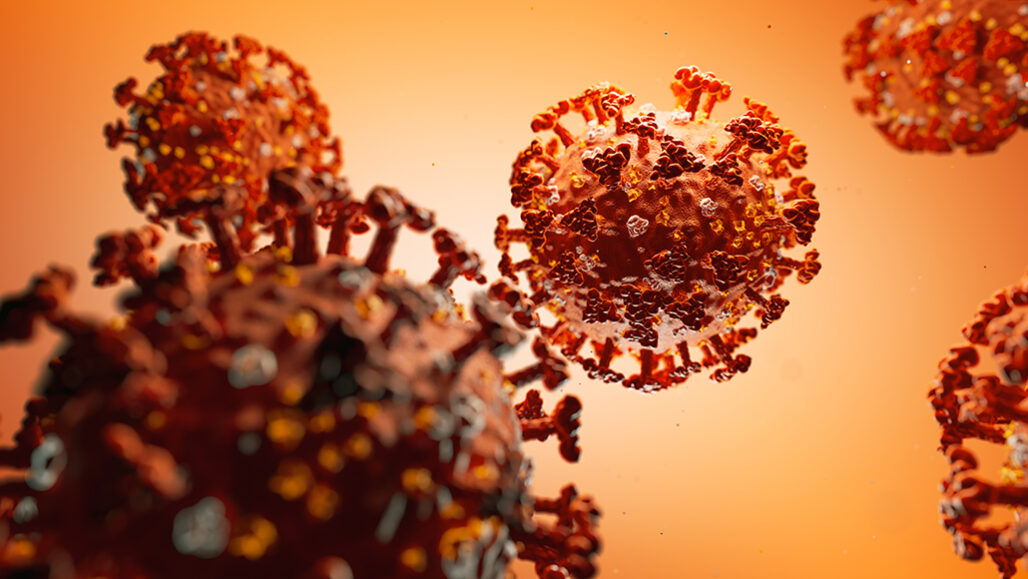
Researchers have confirmed the first known case of someone being reinfected with the new coronavirus (depicted here in artist’s illustration). The 33-year-old man lives in Hong Kong.
Maksim Tkachenko/iStock/Getty Images Plus
A man in Hong Kong has gotten the novel coronavirus — twice. More than four months separated each bout with the virus that causes COVID-19. His is the first confirmed case of reinfection with this virus. If his case is not especially unusual, suggests that some people could be infected again a few months later. This would seem to make a vaccine even more important.
The medical community didn’t know how long people who got sick and recovered might be protected from infection. Every survived infection could bring a community closer to herd immunity. This is where so many people have become infected — and then immune — that the virus can no longer find enough vulnerable people to keep an outbreak going.
In the new case, researchers showed that 142 days after his first infection with the coronavirus, the 33-year-old man was infected again.
Researchers reported his case on August 24. They will share details of their analysis later in Clinical Infectious Diseases. The journal has accepted the study for publication.
Some isolated reports had emerged of people who had recovered from COVID-19 only to once again get sick with the virus. But without genetic data showing that each round of illness had been caused by two different viruses, it was unclear whether such cases were true reinfections. For instance, some common colds are caused by coronaviruses. And people can get infected over and over with these viruses. As our immune response to them wanes, we once again become susceptible to them.
Educators and Parents, Sign Up for The Cheat Sheet
Weekly updates to help you use Science News Explores in the learning environment
Thank you for signing up!
There was a problem signing you up.
Twice infected, but only sick once
The man had a fever, cough, sore throat and headache for three days in March. Late that month he tested positive for SARS-CoV-2. That’s the virus that causes COVID-19. The man was admitted to a hospital in Hong Kong three days later. By then his symptoms were gone. He was released on April 14. That was after he tested negative in each of two separate tests for the virus.
But on August 15, this man again tested positive. He found out when airport officials screened him upon returning to the Hong Kong from Spain. This time, the man showed no sign of being sick. It meant his immune system had kicked in to protect him.
The fact that someone can be reinfected is “not a huge shock,” says Paul Bieniasz. He is a virologist at The Rockefeller University in New York City. (He also works with the Howard Hughes Medical Institute). People often get reinfected with coronaviruses that cause the common cold. And if they don’t mount a strong enough defense, they can get sick that next time.
What’s unknown right now, he says, is “how often this occurs and to what extent.” If reinfections are common, it might make it hard to ever reach herd immunity. Vaccines, however, might trigger a more robust immune response. And that might help from getting infected again.
Overall, it’s unknown how long immunity to SAR-CoV-2 lasts. Some people can test positive for the virus’s genetic material for months after they get well, and shed no infectious virus. A few studies measuring antibodies — key proteins that recognize and bind to germs — suggest that their levels do wane with time. Some coronavirus work hints that antibodies to stop the virus from entering cells may remain in the blood for at least three months.
The latest data, from just one person, might not reflect what usually happens, experts warn. Researchers will need to review more cases to know for sure.
“If you infect five million people with anything, there’s going to be one or two people that [respond] way different than the rest,” says Mark Slifka. He’s an immunologist who specializes in viral diseases. He works at Oregon Health and Science University in Portland.
The virus had changed
Kwok-Yung Yuen works at the University of Hong Kong. This microbiologist was part of a team that sequenced the nucleotides — or building blocks — that make up the virus’s RNA. (Like DNA, RNA is a type of genetic material. It’s the type found in these viruses.)
Viruses from each of the Hong Kong man’s bouts of COVID-19 differed by 24 nucleotides. That indicates that the man was infected with two distinct versions of SARS-CoV-2. One is closely related to types seen in British and U.S. patients in March and April. The second type was seen in Switzerland and England in July and August.
Ten days after the Hong Kong patient first developed symptoms of COVID-19, he tested negative for antibodies to its virus. He may just have had too few for researchers to detect at that time. The next time he got infected, he also didn’t have antibodies on the first three days he was in the hospital. He did, however, show telltale antibodies on day five. By then, his immune system had kicked in to fight the virus.
Although the study shows reinfection can happen, it also suggests that the body revs up to fight off those later infections. Indeed, says Bieniasz, “People shouldn’t think that everybody’s going to be susceptible to infection within four months.”
No one knows how often reinfections with the new coronavirus might be happening, especially if symptoms are milder or absent the second time. “When we say that people don’t typically get reinfected, that’s based on . . . when people get sick again,” Slifka says. If they don’t appear sick, they may be infected and no one would know.
It’s also not known if the Hong Kong man could spread his second virus. That ability to spread is important, says Kartik Chandran. He’s a virologist at Albert Einstein College of Medicine in New York City. “Some people will still develop some sort of infection.” But if their bodies mount a strong immune response, he notes, “they may not get seriously ill,” yet still infect others. It’s also possible, he adds, that the second time around, someone may not spread any virus.