Explainer: What is RNA?
A partner to DNA, this molecule translates genetic instructions to make proteins
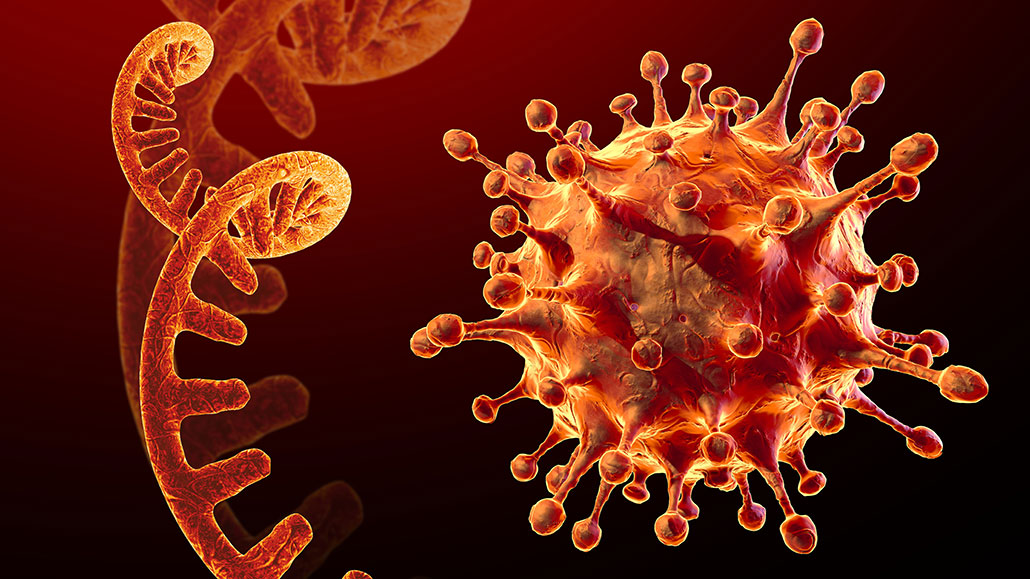
Its protein-making skills make RNA a major player in our immune systems. Here, a single strand of RNA (left) from the coronavirus is illustrated alongside a SARS-CoV-2 virus particle (right).
CROCOTHERY/iStock/Getty Images Plus
DNA is the genetic material that serves as our body’s genetic blueprint. DNA is short for deoxyribonucleic (Dee-OX-ee-ry-boh-nu-KLAY-ik) acid. It tells cells how to make all the proteins that will be needed for the body to survive. DNA receives a lot of attention, but it wouldn’t work without a key partner: RNA. That’s short for ribonucleic (RY-boh-nu-KLAY-ik) acid.
To understand the DNA-RNA partnership, imagine an instruction manual titled How to Build a Car. The manual shows the proper steps to build a car, but just having that book won’t produce a car. Something, or someone, must carry out the labor. RNA performs that action for cells. It puts the information stored in DNA’s twisting, ladder-like shape to use.
Proteins are the body’s workforce. They carry out the specialized, molecular-level tasks in all living things. Our blood moves life-sustaining oxygen to cells throughout the body. To do this, it uses the protein hemoglobin. Our digestive system breaks down what we eat into usable bits using other proteins. For instance, amylase (AA-mih-lays), a protein in saliva, breaks the starch in breads and potatoes down into sugars. Our bodies are built from many types of molecules, and it uses specific proteins that make those molecules.
To know which proteins to make, when to make them and where, the body relies on its instruction manual, DNA. RNA follows those instructions to make proteins. But RNA isn’t just one molecule. Here we focus on three major types.
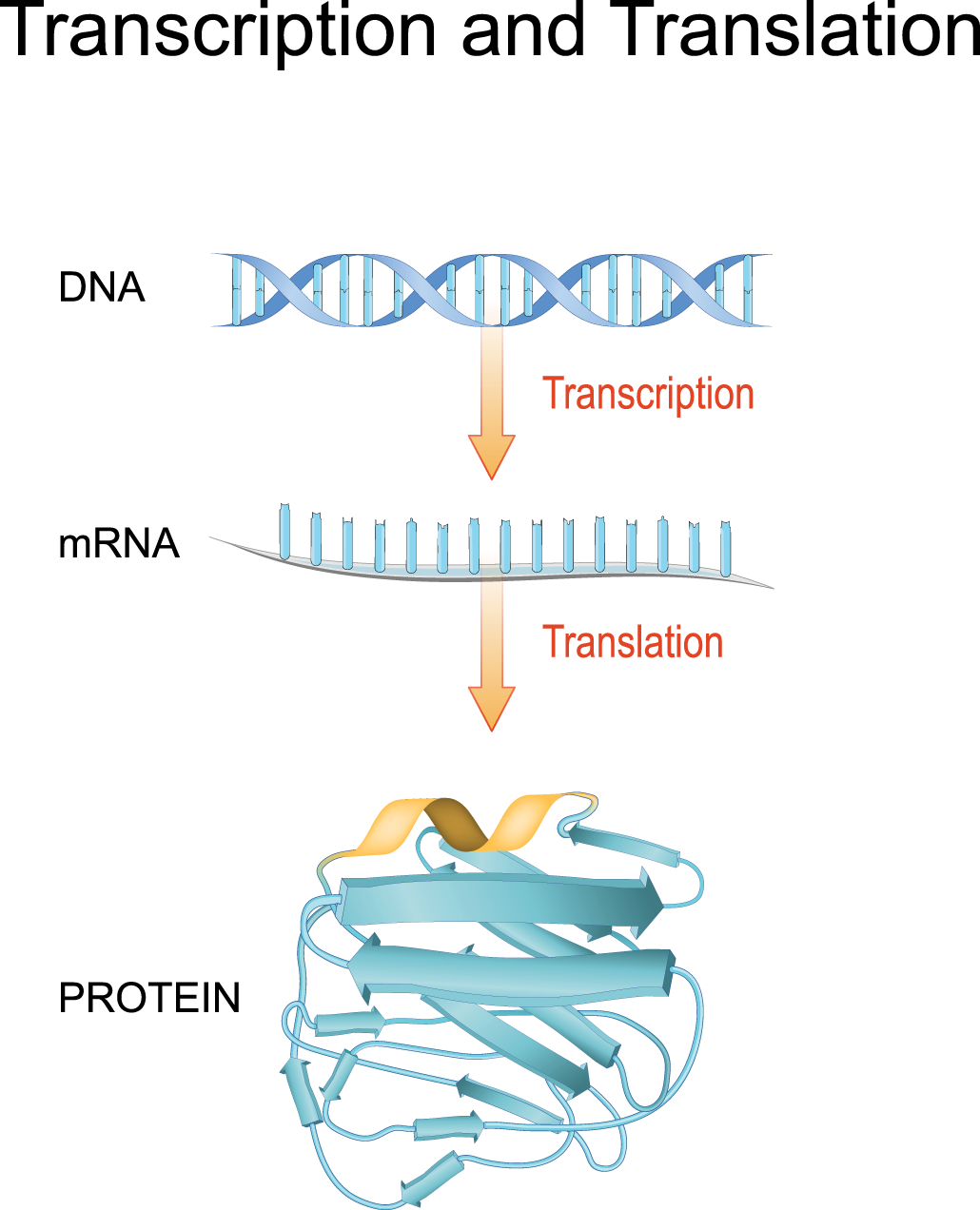
mRNA: Protein creation starts inside a cell’s nucleus. That’s where the DNA sits. A cell copies DNA’s instructions — a process scientists call transcription — onto a strand of messenger RNA, or mRNA. It’s a good name, because mRNA is a message. Once created, it exits the nucleus, leaving the DNA safe inside.
rRNA: Outside a cell’s nucleus, the mRNA binds to what’s known as rRNA. That’s short for ribosomal (Ry-boh-SOAM-ul) RNA. Its job is to decrypt the message in mRNA and use that information to build a new protein. Proteins are made of subunits called amino acids. rRNA snaps amino acids together in the proper order. rRNA wouldn’t know the right order without mRNA, so they work as a team. This step is called translation.
tRNA: Transfer RNA, or tRNA, acts like a taxi. It ferries amino acids from areas throughout the outer portions of a cell (its cytoplasm) over to the builder-molecule: that rRNA.
Together, this RNA trio works together to create the proteins living things need to function.
RNA viruses and vaccines
RNA has gotten a lot of attention in the last couple of years. In 2020, COVID-19 turned a spotlight on RNA. Viruses are not cells. They do, however, carry their own genetic instruction books. The coronavirus responsible for COVID-19 is an RNA-based virus. That means its genetic instruction book is made from RNA, not DNA.
And the first vaccines approved to fight COVID-19 were a new type: They focused on mRNA. It makes sense that RNA plays a role in immunity. The body’s immune system launches specialized proteins to fight off germs. In 2020, scientists working for a drug company known as Pfizer developed the first RNA vaccine that would go on to receive full approval from the U.S. Food and Drug Administration. One or more other RNA vaccines could be approved soon.
Vaccines work by tricking the immune system into thinking a pathogen is present. The immune system now mounts a defense. It dispatches an army of troops to circulate throughout the blood and track down more invaders. However, even after a pathogen — or an imposter (vaccine) — is gone, our bodies remember what the invader had looked like.
The immune system can remain on high alert scouting for that pathogen. If it appears once more, the body identifies it by its unique external features, called antigens. Then the immune system again mounts an immediate defense. Usually, this rapid response kills off the pathogen before we were even aware it had invaded the body.
Educators and Parents, Sign Up for The Cheat Sheet
Weekly updates to help you use Science News Explores in the learning environment
Thank you for signing up!
There was a problem signing you up.
A traditional vaccine works by exposing the body to a pathogen (usually killed or weakened) or pathogen look-alike. Even a dead pathogen can trigger an immune response because it still has the antigens on its surface that alarm the body’s defense troops. If the real pathogen later reappears, the vaccine is ready — primed — to attack.
mRNA vaccines work differently. Instead of introducing a pathogen or look-alike, mRNA vaccines pass on the mRNA instructions for making one of the pathogen’s antigens — and only that antigen. But that’s enough for the body to learn what to look out for. For the COVID-19 vaccine, those mRNA molecules give the body instructions that help it scout for signs of the virus’s spike protein.
“When that mRNA gets into our cells, it then produces over and over again copies of that spike protein,” explains Gregory A. Poland. He’s a vaccine scientist at the Mayo Clinic in Rochester, Minn. That particular spike protein is found only on the outside of the virus that causes COVID-19.
Once someone receives a shot of an mRNA vaccine, the rRNA and tRNA in their cells start translating the vaccine’s mRNA into a protein — the antigen. That tricks the immune system into thinking the virus has infected the body. In that way, the vaccine gets the body to develop the defensive troops it needs to hunt down and kill the real coronavirus if and when the real virus shows up.