Chikungunya wings its way north — on mosquitoes
The tropical scourge has adapted to survive in mosquitoes that thrive in the United States and other temperate zones
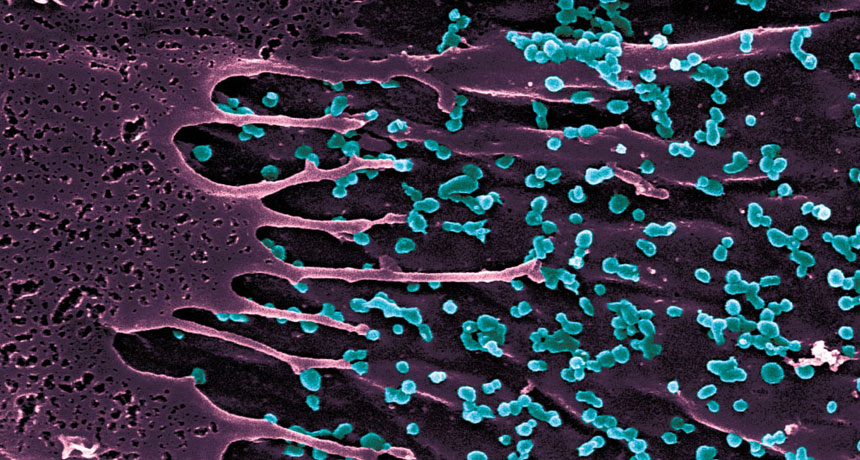
Blue-stained dots are Chikungunya virus particles peppering the surface of an infected cell.
© Institut Pasteur/Thérèse Couderc
By Nathan Seppa
A crippling virus has escaped Africa and Asia. Now it’s invading other continents faster than people can learn to pronounce its name. The virus, carried by mosquitoes, causes chikungunya (Chihk-uhn-GUHN-yuh) fever. And in just 10 years, it has gone from an obscure tropical disease to a worldwide threat. So far it has caused more than 3 million infections around the globe. The virus recently took root in Latin America. It may now be able to inflict misery in cooler climates, including North America.
Chikungunya rarely kills its victims. But it can bring a world of hurt. It begins like the flu — fever, chills, headache, aching joints. And it typically lingers for a week. But for many people, that is far from the end of it. Over time, severe joint pain can emerge. And that pain can linger for months — even years. The virus causes many of its victims to have a stooped posture. Indeed, in a tribal language of East Africa, chikungunya means “to walk bent over” or “to become contorted.”
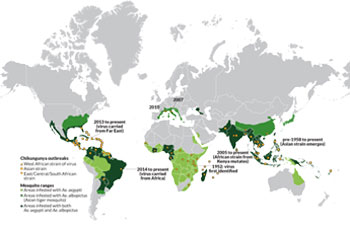
The mosquito-borne virus has ventured from its home in Africa several times. It settled into Southeast Asia in the 1950s. But most of its other attempts to escape Africa fizzled.

It’s not the first time a tropical disease has reached other warm regions. But usually such diseases don’t spread to cooler regions outside the tropics, called temperate zones. Now, one strain of the chikungunya virus has found a way to survive in mosquitoes that live in those cooler zones. That allowed it to recently spread into Italy and France. North America, China and Europe could be next.
So chikungunya could be coming to a mosquito near you. No one knows whether the virus will be able to become deeply rooted in temperate zones. But U.S. outbreaks are a real possibility, says Stephen Higgs. He’s a chikungunya expert at Kansas State University in Manhattan.
Island hopping
The sleepy island of Réunion is a French territory in a remote part of the Indian Ocean. It sits off of the southeast coast of Africa. This would seem like an ideal place to avoid global health problems. But in 2005 and 2006, chikungunya arrived there from the mainland.
The disease devastated Réunion. Some 266,000 of the island’s roughly 800,000 people were struck. At the height of the outbreak, 40,000 patients a week streamed into clinics there. The virus also blew through other islands in the region. When it got to India in late 2005, chikungunya hit the jackpot — close to 1.4 million infections. From India it spawned outbreaks across Southeast Asia.
This explosion of infections stunned global health experts. Something had changed.
Réunion seemed an odd stopover for the virus. That’s because the island had few if any Aedes aegypti (AY-dees Eh-JIP-tye) mosquitoes. These are the tropical mosquitoes that typically carry the virus around Africa and Asia. But as in many cooler parts of the world, another type of mosquito swarms across Réunion: Aedes albopictus (AL-boh-PIK-tus). It many places, this black-and-white-striped blood sucker is known as the Asian tiger mosquito.

When a mosquito takes a blood meal from a person carrying chikungunya, the virus quickly makes many copies of itself in the insect’s gut. That process is called replication. The newly formed viruses then travel to the mosquito’s saliva. As a result, the insect’s next bite is like a hypodermic needle loaded with virus.
Until the virus mutated, tiger mosquitoes couldn’t spread chikungunya very well. But the new mutation made it about 100 times easier for the virus to survive inside the tiger mosquito’s innards long enough to replicate. The next time that mosquito bit someone, it now could shed some of the virus to its victim.
Jets bound for cooler climates sometimes took off with passengers who had been bitten by tiger mosquito. It should come as no surprise, then, that within a few years some infected visitors brought chikungunya with them to Italy and France. Italy reported about 200 infections in 2007.
That’s not a very big number. Still, it showed that chikungunya could successfully venture outside the tropics. “That was a game changer,” says Scott Weaver. He’s a virus expert, or virologist, at the University of Texas Medical Branch in Galveston.
Westward ho!
A second surprise came in 2013 when chikungunya showed up on the sun-splashed Caribbean island of Saint Martin. It lies about 2,000 kilometers (1,242 miles) southeast of Miami. A traveler arrived there carrying the virus. Scientists believe this infected visitor arrived from Asia. On the island of Saint Martin, this traveler was then bitten by a local mosquito.
Clearly, Weaver says, “Our luck ran out.” In the next year and a half, chikungunya found a foothold in the Americas. And it may never go away. Florida had 11 cases in 2014. All were transmitted by local mosquitoes. The warm states bordering the Gulf of Mexico also may be at risk. The reason? Aedes aegypti, the tropical mosquito that appears to be driving the epidemic, can live there, explains Higgs at Kansas State. He adds that the reason the Caribbean infections haven’t spread further into North America is because those mosquitoes can’t survive in the colder states.
But the tiger mosquito can. If a sick traveler were to bring chikungunya to Europe or the eastern United States, the disease would not spread — unless the traveler was carrying a strain of the virus adapted to the tiger mosquito.
Meanwhile, Aedes aegypti is spreading the Asian strain of chikungunya in Latin America and the Caribbean. Tens of thousands of cases have been confirmed. More than 1 million people are suspected of having become infected. This epidemic has stretched to Brazil in the northernmost part of South America. There, the virus has spread the disease from person to mosquito to person — hundreds of times.
Much of Brazil is home to both the tiger mosquito and Aedes aegypti. Scientists now are trying to determine which insect is spreading the virus there. Brazil has a second problem. It has cases of both strains of chikungunya — the Asian strain that swept the Caribbean and the African strain that learned to ride the tiger mosquito in the Indian Ocean.
Researchers don’t know yet if the African strain has mutated in Brazil as it did in Réunion.
If the virus in Brazil does mutate, the West could face a worst-case scenario. That’s because Panama, Mexico and many other countries also have both mosquitoes. The risk posed by having a version of chikungunya in the West that has adapted to cooler-zone mosquitoes keeps U.S. infectious disease experts up at night.
“It’s certainly something I worry about,” says Mark Heise. He’s a virologist — a scientist who studies viruses — at the University of North Carolina at Chapel Hill.
Oh, the pain
People rarely get chikungunya twice. But once is bad enough.
The CDC’s Ann Powers first saw people sick with chikungunya in the Comoros. It’s a group of islands in the Indian Ocean. These islands were hit about the same time as Réunion was. Powers interviewed some patients as they lay down. Their ankles were so inflamed they couldn’t stand. “Shaking hands hurt them,” she says. “It was incredible to see people in that much pain,” she says.
One long-term program monitored 102 patients in Réunion. It found that three years after being infected with the chikungunya virus, 60 percent still reported joint pain. A French team reported those findings in the scientific journal PLOS Neglected Tropical Diseases in 2013. In Italy, nearly 67 percent of patients continued to have pain a year after first becoming infected.
The crippling joint symptoms can disable a whole community, says David Morens. He works at the National Institute of Allergy and Infectious Diseases in Bethesda, Md. He specializes in studying viruses and other germs that affect children. “In Asia,you see these really massive outbreaks where everybody gets sick at once.” Before long, he notes, “There are no taxicabs, no teachers.” Everyone seems to have gotten sick.
Pregnant women face special risks. Of 39 pregnant women in Réunion who had chikungunya fever around the time they were about to give birth, 19 had infected newborns. And 10 of those infants developed serious health problems, French researchers reported in 2008.
Treatment options are limited
There are few treatments for chikungunya. Doctors can offer drugs to reduce fever and provide fluids to limit the risk of dehydration. The drug ribavirin, which stops some viruses from replicating, also appears to help somewhat.

One 2013 study used mice. It found antibodies from mice that survived the disease could block chikungunya virus from infecting new animals. The antibodies even worked when injected after the virus had infected mice — as long as they did not yet show symptoms, says Heise at the University of North Carolina. His team authored the report, published in PLOS Pathogens.
Researchers also think it might be possible to stop chikungunya by using the body’s natural immune response against it. They’d do this with a vaccine. Several research teams have reported promising results from vaccines that use chikungunya proteins. These viral bits kick-start the production of antibodies that can block infection.
In one study, a vaccine made from the virus’s own proteins gave people protection for at least 44 weeks. That study was led by Julie Ledgerwood. She’s a vaccine researcher at the National Institute of Allergy and Infectious Diseases in Bethesda, Md. Her team reported its results in the December 6, 2014, issue of a medical journal, The Lancet.

If the chikungunya virus finds ways to survive in temperate regions, like most of the United States, infections there could become an annual summertime risk, says Powers of the CDC.
Others doubt chikungunya will linger in the West. In the past, chikungunya may have escaped Africa every 50 or 60 years. Each time, it flared for a while and then died out, says Scott Halstead. He’s an infectious disease physician at the Uniformed Services University of the Health Sciences in Bethesda, Md. He doubts the virus will spread permanently to all parts of the globe.
For the virus to stay in the West, it has to either adapt itself to humans or to wild animals, says Morens of the National Institute of Allergy and Infectious Diseases. If it infects monkeys, chikungunya could linger under the radar for years at a time. Then, now and again, it could cross over into people. This is what chikungunya — and Ebola — both do in Africa.
“The other possibility is more alarming,” Morens says. “The virus adapts itself to a new cycle, completely human-to-mosquito-to-human.” It might evolve in a way that no longer needs a long-term wild-animal host. If that happens, he says, “it’s almost never going to go away.”
Word Find (click here to enlarge for printing)