Five questions about COVID-19 vaccine trials in teens, answered
From trial safety to how you can sign up
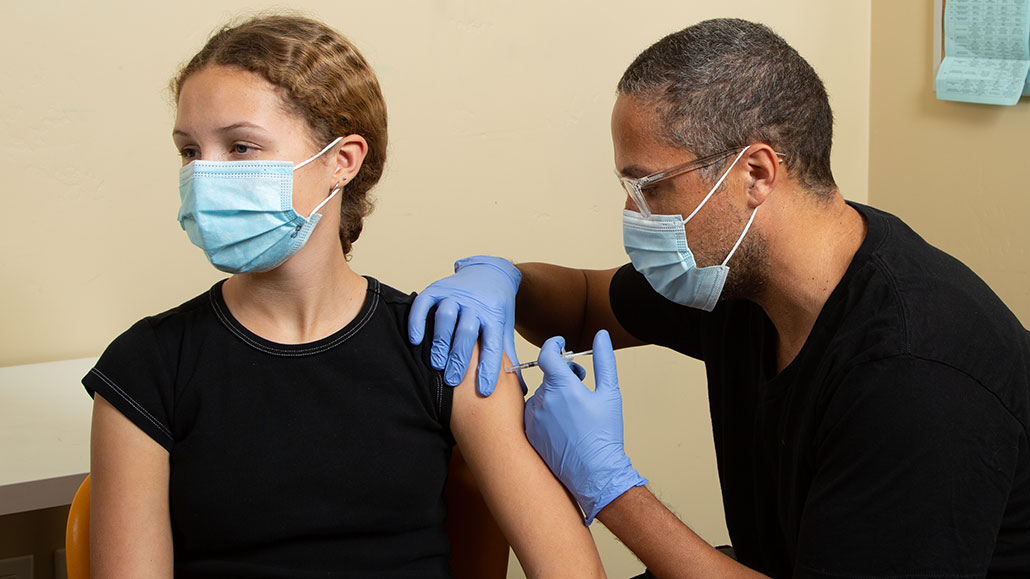
Teens aren’t eligible for the COVID-19 vaccine yet. But they can volunteer for clinical trials.
Side Show Stock/iStock/Getty Images Plus
COVID-19 vaccines are now being distributed across the United States. But most teens can’t get one. Kids under 16 don’t yet qualify for the vaccine. That’s because, so far, the vaccine has only been tested in adults. Now, Moderna and Pfizer, the makers of the two vaccines being given to adults, are running clinical trials in teens and kids. These trials will help scientists figure out if the vaccines work in young people as they do in adults.
Pfizer has recruited more than 2,000 kids ages 12 to 15 for its trial. However, Moderna reports having trouble recruiting the 3,000 12- to 17-year-olds needed for its trial. Volunteering to take a mystery shot for science can definitely give parents and teens pause. Here are five questions that teens and parents might have.
How does the vaccine compare to the ones in adults? Is it safe?
Emma Bardon wanted to know if her child, Katie, would get the same dose of vaccine that an adult might.
“Both the clinical trials that are accepting children 12 years and older are using the exact same vaccine at the same dose and at the same interval,” says Jill Weatherhead. It’s “identical to what they’re doing in the adult trials.” Weatherhead is a pediatrician, a doctor who works with kids. She also studies infectious disease at Baylor College of Medicine in Houston, Texas.
For her part, Katie Bardon, 12, wanted to know if people might have allergies to the vaccines. Katie is in 7th grade in Canada at Edenwood Middle School in Mississauga, Ontario.
Clinical trials are designed to find side effects and allergies, explains Evan Anderson. He’s a pediatrician and vaccinologist — someone who studies vaccines — at Emory University School of Medicine in Atlanta, Ga. He’s been part of the clinical trials for Moderna and Johnson & Johnson. If a teen joins a clinical trial, he says, scientists will be looking for everything from a sore arm to a bad reaction that might send someone to the hospital.
Some side effects are expected, Anderson notes. And that’s not unusual for a vaccine. Consider the flu vaccine. “When people talk about ‘getting the flu from the flu vaccine,’” he says, they’re not actually getting the flu. A person might experience a fever, chills or a headache after the getting the shot. But that’s only their immune system “turning on.” And when it comes to the COVID-19 vaccines, he notes, “We see similar turning on for the immune system.” Common side effects include a sore arm, aches and chills.
Educators and Parents, Sign Up for The Cheat Sheet
Weekly updates to help you use Science News Explores in the learning environment
Thank you for signing up!
There was a problem signing you up.
Why do scientists need to do separate tests in teens?
Age does matter for vaccines. When babies are less than one year old, for instance, “their immune system hasn’t developed yet,” Weatherhead explains. “As you age … that immune system is revving up and learning and developing and getting stronger.” By the time people reach their teens, she says, “there shouldn’t be a huge difference between a teenager and a young adult.”
When kids are younger, they’re also smaller. So they might end up needing less vaccine to keep them safe, says Anderson. “It’s possible that as we get to …12 to 15 [year olds], they might not need as much of a vaccine as older and more fully developed teenagers,” he says. The tests are also important to make absolutely sure the vaccine is as safe in kids and teens as it is in adults.
What would happen if I volunteered for a vaccine trial?
If a teen is selected to participate in a trial, they’re placed in one of two groups. One group receives the vaccine. The other group gets a placebo — a shot with no effect at all. The placebo group allows the scientists to determine if and how well the vaccine works. Each group would get another shot of either vaccine or placebo three to four weeks later, just as in trials with the adult vaccines for COVID-19.
“We collect a lot of information around the time of each dose,” Anderson says. The scientists want to know everything that a person experiences when they get the shot, so they can detect any harmful effects. If anything did happen, he notes, the trial would stop immediately, and the teens and parents would be informed.
Safety is a major concern. Clinical trials are designed with safety in mind, says pediatrician Douglas Diekema. He works at Seattle Children’s Hospital in Washington. As a bioethicist, he studies codes of conduct in biology and medicine. Because kids can’t fully consent for themselves, he notes, scientists make sure the vaccine is safe in adults first. Diekema is the head of something called an Institutional Review Board (IRB) that reviews scientists’ clinical trials. “Our job is to make sure that a clinical trial like this does not expose children to risks that aren’t justified by the benefits of being in the clinical trials,” he explains. “The IRB isn’t even going to allow this trial if they think the risks to kids are excessive.”
After the trial begins, Weatherhead notes, scientists and doctors keep checking the results for safety. “We’ve seen that in the AstraZeneca trials and in the Johnson & Johnson trials,” she says. (Those trials have tested vaccines that have not yet been approved for use in the United States.) When someone got sick in the AstraZeneca trial, “they shut down the whole trial for one event. It’s taken very seriously,” she says. When the illness turned out not to be due to the vaccine, the trial started again. And the vaccine worked.
Some parents are concerned about what data might be collected on their kids. “The key thing to mention up front is that parents and teens are going to need to provide consent,” says Anderson at Emory. Everyone needs to read and understand the terms of the trial. The consent forms usually describe what data the study will collect. For COVID-19 vaccine trials, he notes, scientists will collect data on medical history, whether the teen or their close contacts has had COVID-19, other vaccines they’ve had and when and what medications they take.
Another important thing is privacy. “Everybody gets a study number,” Anderson says, “Then all their information is put into the main study with their number. There’s no direct identifying information.” That way other people who see the trial results won’t be able to identify the teens who took part.
How do I decide if I want to participate?
Some teens are eager to volunteer “because they want to contribute,” Diekema says. “It’s so heartwarming to hear it from some kids.” But every trial does have risks, he cautions. So it’s important that anyone interested in participating read about the trial, talk to their doctor and weigh the benefits and risks.
“We don’t know for sure there won’t be some rare things that happen six months from now,” Diekema says. “Is that likely? No. But almost every vaccine has these rare things that happen in one out of 1,000 or one out of 1 million patients.”
Also, anyone participating needs to understand that they might not get the vaccine. They could get a placebo. An important question to ask, Diekema says, is “’How soon can I get this vaccine after it’s approved in my age group if I’m in the placebo group?’”
Anderson, Weatherhead and Diekema are all parents. Weatherhead’s and Diekema’s kids are either too young or too old for the trials. Because Anderson runs some clinical trials, his kids aren’t allowed to enroll. “I would love for my kids to be able to, actually,” he says. “Several of them are interested.”
Weatherhead and Diekema would also be fine with their kids participating if that were possible. Based on how effective the vaccines are, and how mild the side effects are, “when it comes time for my kids’ age group, I would have them receive it too,” Weatherhead says.
Twelve-year-old Katie says, “I would take part in the trials if it was okay with my parents.” The trials aren’t enrolling teens where she lives. But she still wants to participate “so children who are at risk could have the vaccine and get better and so they could reopen schools. I like seeing my friends,” she says.
Bardon, Katie’s mom, says it would be fine with her, too. “I know there’s a lot of safety information available,” she says. “As long as there’s information to review before enrolling, I’m pretty comfortable.”
If I do want to participate in a trial, what should I do?
Often, the hardest part about getting into a COVID-19 vaccine trial is finding one. In some cases, a teen’s doctor might know whether trials are going on nearby.
The National Institutes of Health has a site called clinicaltrials.gov. This is where every clinical trial testing a drug or device in the United States is required to be registered. The COVID-19 vaccine trials are listed there, and the page for each one (Moderna and Pfizer) includes a list of locations where the vaccine is being tested. Interested people can contact those locations to find out if they can sign up. Many won’t end up qualifying, however.
“Having [teens] be part of this process is really important.” Weatherhead says. “They’ve sacrificed so much. They can’t do extracurriculars, can’t see their friends. Of all the age groups that needs normalcy and routine, these kids deserve that.”







